We used to think of chronic diseases like a one-way street. You get the diagnosis, you take the pill, and you manage the decline. That's a reactive mindset. Today, we're talking about lifestyle medicine. It's a shift from just treating symptoms to using your daily habits as the primary clinical intervention. The latest 2025 guidelines from major groups like the American Heart Association and the American College of Lifestyle Medicine have officially categorized lifestyle changes as Class I, Level A interventions. That's the gold standard. It means these changes aren't just "nice to have" or "supportive care." They're the most effective tools we have to stop, and sometimes even reverse, the progression of disease.
Type 2 Diabetes Reversing the Pre-Diabetic Trajectory
Have you ever been told your blood sugar is "a little high"? That's often the first sign of insulin resistance, and it's your biggest opportunity to change the future. We used to view Type 2 Diabetes as a lifelong, progressive sentence. New data from 2024 and 2025 has completely flipped that script.
The 2024 extension of the DiRECT study, published in The Lancet, showed us something incredible. About 13% of people who went through intensive weight management were still in full remission five years later. They didn't just "manage" their diabetes. Their blood sugar returned to normal ranges without any medication.
The magic number seems to be around 9kg, or 20 pounds. People who maintained that level of weight loss had the highest success rates in keeping the disease at bay. It's about giving your pancreas a break and letting your cells become sensitive to insulin again through whole-food, plant-predominant nutrition and consistent movement.
Cardiovascular Health
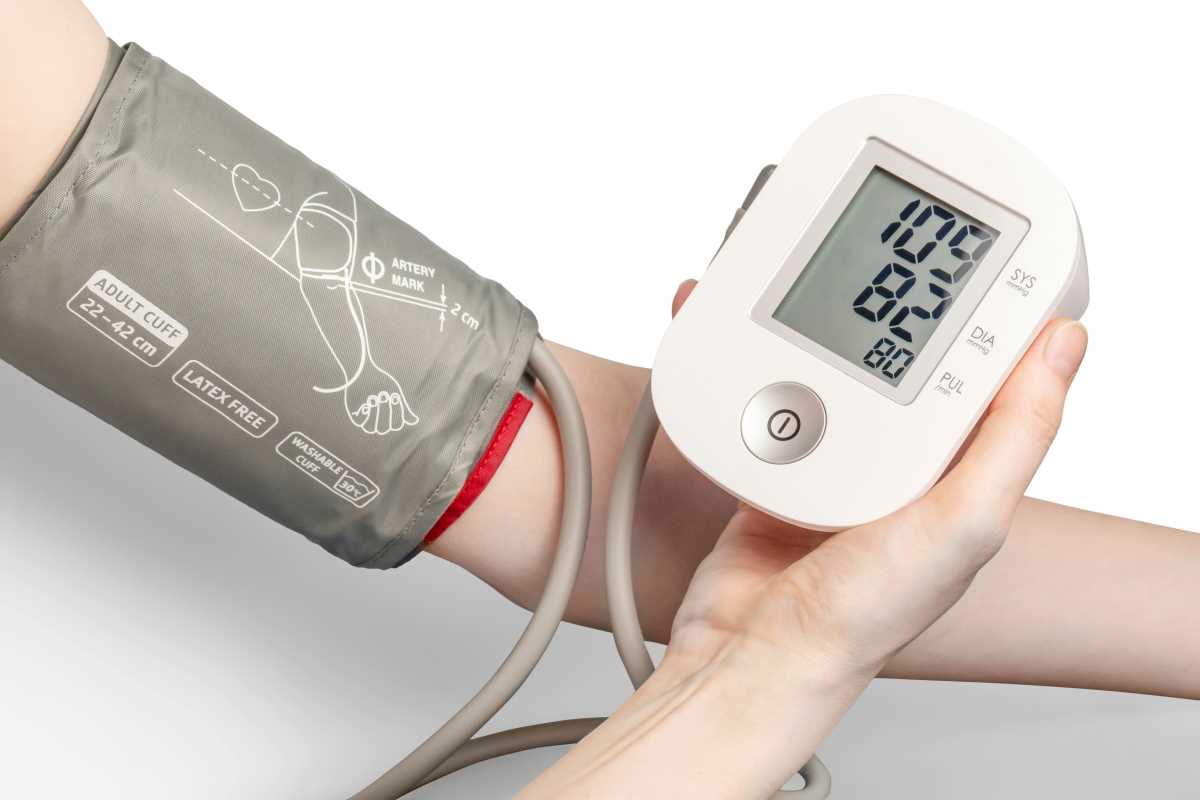
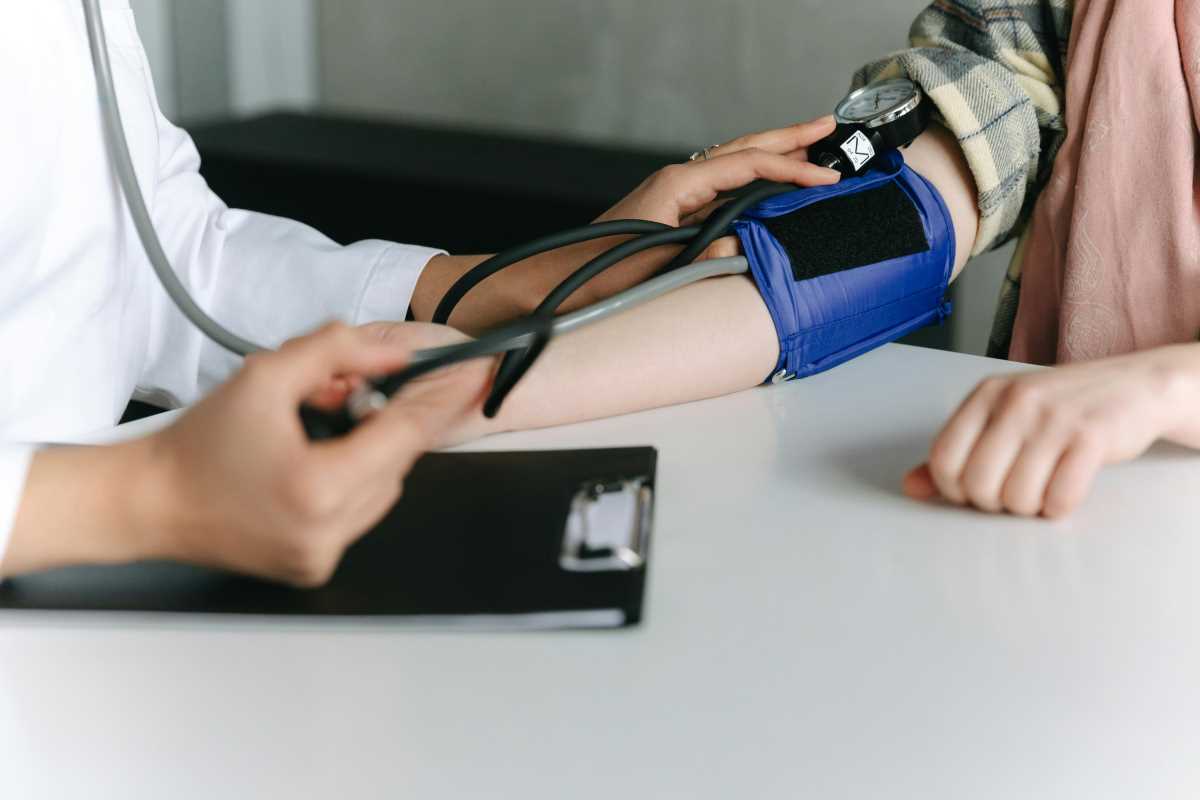
Heart disease is often called a silent killer because you don't feel your arteries hardening. But your blood pressure and cholesterol levels are telling a story long before a heart attack happens. If you're seeing early signs of hypertension, you have a window of time to act before your heart takes permanent damage.
The 2025 guidelines for blood pressure introduced the "1-for-1" rule. It's a simple way to look at it: for every kilogram of weight you lose, your systolic blood pressure typically drops by 1 mmHg. If you lose five kilograms, that's a 5-point drop. That is often enough to move someone from "at risk" back into the safe zone.
It's not just about weight, though. The 2024 European Society of Cardiology guidelines moved sodium restriction and potassium intake to their highest recommendation level. Switching to a DASH-style diet, which focuses on fruits, veggies, and lean proteins, can lower your blood pressure as much as a standard prescription drug. It's like giving your vascular system a tune-up every time you eat.
Managing Autoimmune Inflammation Through Lifestyle
If you struggle with joint pain, skin issues, or constant fatigue, you might be dealing with systemic inflammation. This is often the precursor to autoimmune conditions. Although genetics plays a role, your environment and lifestyle are the "on" switches for these genes.
Your gut health is the front line of your immune system. When your microbiome is out of balance, it can trigger inflammatory responses throughout your body. Early lifestyle shifts like increasing fiber and reducing ultra-processed foods can help calm this internal fire.
Sleep and stress are the other two legs of the stool. A 2025 study from the UK Biobank found that irregular sleep, especially going to bed after 12:30 AM, significantly increases the risk of chronic inflammatory diseases.² Your body needs that consistent downtime to regulate the immune system. Without it, your defenses stay on high alert, attacking things they shouldn't.
The Link Between Mind and Body
We often separate mental health from physical health, but the science in 2026 says they're the same thing. Have you ever noticed how your stomach ties in knots when you're stressed? That's not in your head. It's a physiological response that drives up inflammation.
A 2024 study from Ohio State University found that inflammation explains over 60% of the link between stress and metabolic syndrome.³ When you're constantly "on," your body produces cortisol, which messes with your metabolism and your mood. It's a vicious cycle that lifestyle medicine is uniquely equipped to break.
The CALM trial, a world-first study published in 2025, proved that structured lifestyle therapy is just as effective as traditional psychotherapy for relieving depressive symptoms.¹ This doesn't mean you shouldn't see a therapist. It means that what you do with your body - how you move and what you eat - is a powerful antidepressant in its own right.
Top Recommendations
If you're looking to get started with lifestyle medicine, these are the areas where you'll see the biggest "bang for your buck" based on the latest research.
- Prioritize Sleep Regularity: Aim for the same bedtime every night. Research shows that consistency is often more important than the total number of hours for preventing chronic liver and metabolic issues.²
- Focus on Plant-Based Proteins: You don't have to go full vegan, but swapping animal protein for beans, lentils, or tofu a few times a week reduces the workload on your kidneys and lowers inflammation markers.
- The 10% Weight Goal: If you're dealing with fatty liver (MASLD) or early-stage diabetes, aim to lose 10% of your body weight. This is the threshold where we see actual reversal of liver scarring and disease remission.
- Move Every 30 Minutes: You don't need a marathon. Replacing just 30 minutes of sitting with light walking throughout the day can cut your cardiovascular risk by up to 20%.
Getting Started
So what does this actually mean for you? It means you have more power than you think. But the biggest mistake people make is trying to change everything on a Monday morning. That's a recipe for burnout.
Start with "small wins." Maybe this week, you just focus on drinking more water and hitting a consistent bedtime. Next week, you will add a 15-minute walk after dinner. These small habits stack up over time. What matters is being consistent enough to change your internal chemistry.
Track your progress, but don't just look at the scale. Look at your energy levels, your sleep quality, and your blood work. Work with a healthcare provider who understands lifestyle medicine. They can help you monitor your markers and adjust your plan as your body begins to heal.
Taking ownership of your health journey is the most helpful thing you can do. The "prescription" for a longer, healthier life isn't always found at the pharmacy. Sometimes, it's found in your kitchen, on your walking path, and in the quiet moments of rest you give yourself every night.
This article on SuperHealthyTips is for informational and educational purposes only. Readers are encouraged to consult qualified professionals and verify details with official sources before making decisions. This content does not constitute professional advice.
 (Image source: Gemini)
(Image source: Gemini)